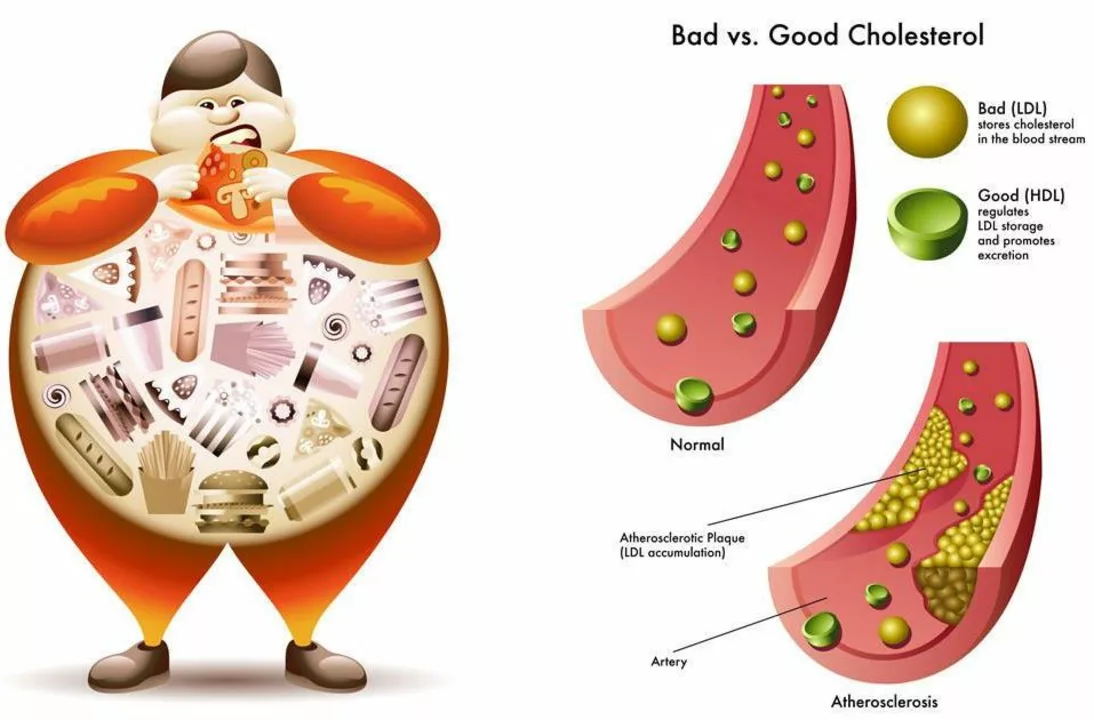
Low-Density Lipoprotein (LDL): What It Means and How to Lower It
Ever gotten a cholesterol result and felt confused by LDL? That’s the one doctors call the "bad" cholesterol because high LDL helps plaque build up in your arteries. Plaque narrows arteries and raises the risk of heart attack and stroke. Knowing your LDL number makes it easier to take real steps to protect your heart.
What the numbers mean
Most labs report LDL in mg/dL. Here are common ranges you’ll see:
- Optimal: <100 mg/dL (for most people).
- Near optimal/above optimal: 100–129 mg/dL.
- Borderline high: 130–159 mg/dL.
- High: 160–189 mg/dL.
- Very high: ≥190 mg/dL — this usually needs strong treatment and close follow-up.
People with known heart disease or diabetes often aim for even lower targets (for example, <70 mg/dL). Your doctor will set a target based on your overall risk.
How LDL is measured and what to watch for
LDL usually comes from a standard lipid panel. Labs often calculate LDL using a formula (Friedewald); it’s less accurate if triglycerides are high. If your triglycerides are above 400 mg/dL, your clinician may order a direct LDL test. You don’t always need to fast anymore—many clinics use non-fasting panels unless your provider asks for fasting results.
So what can you do if your LDL is high? Start with things you can control:
- Diet: Swap trans fats and many processed foods for whole foods. Cut back on saturated fats (fatty red meat, full-fat dairy) and add soluble fiber (oats, beans, barley, psyllium). Try plant sterols/stanols (about 2 g daily) — they help lower LDL by a few percentage points.
- Move more: Aim for 30–60 minutes of moderate exercise most days. Walking, cycling, or swimming help raise HDL and can lower LDL modestly.
- Lose excess weight: Losing even 5–10% of body weight often improves cholesterol numbers.
- Quit smoking and limit alcohol: Both steps help heart risk beyond cholesterol itself.
If lifestyle changes aren’t enough, medications work very well. Statins are first line — they can cut LDL 20–55% depending on dose. Other options include ezetimibe, bile-acid sequestrants, and newer PCSK9 inhibitors for people at very high risk. Your doctor will discuss benefits, side effects (like muscle aches with statins), and monitoring schedules. Usually labs are rechecked 4–12 weeks after starting therapy, then periodically.
If your LDL is ≥190 mg/dL, or you have heart disease, diabetes, or multiple risk factors, see your clinician sooner. Want a simple start today? Add a bowl of oats, take a brisk 20-minute walk, and book a lipid check. Those small steps move the needle more than you might think.